Continuing my posts on excess deaths in Germany, UK, and other vaxxed-to-the-max countries. Here I try to pull some different strands together and weave a better picture of what we know (and don’t know) about the unseasonal and excessive numbers of deaths we are currently seeing around Europe and elsewhere. Here, some key quotes from earlier posts:
The German Federal Statistic Office (Destatis) has released provisional deaths data for last year, and 2022 was a very bad year indeed. Monthly figures had been released throughout the year so it was no secret 2022 consistently featured excess mortality. Almost every weekly total was above the 2018-2021 median and every monthly total since April was above the 2018-2021 maximum. Surprising however is the total number of deaths for December which reached a German record high of 111,403 for a single month. This pushed the yearly total for 2022 to over 1 million, to also a new German record high.
Is the pandemic even really over if German deaths have continued to climb and are currently surging?
…one of the many curious aspects of the pandemic is the near global disappearance of influenza during the pandemic winters 2020/21 and 2021/22 only to resurface in early 2022 just as SARS-Cov-2 was apparently receding…
Because calculations of excess mortality are dependent on expected deaths, changes in flu season patterns and associated deaths will affect expected deaths and can affect year-on-year comparisons made for individual weeks, months, or calendar years. This is one reason why it is preferable to center the mortality year around a single winter for better comparability and why we need to wait for the death figures for the remaining winter months to make any definitive proclamations about the excess mortality we are currently witnessing this winter.
In a weird way, public health in many nations did manage to “flatten the curve”. No, I don’t mean they dampened the initial waves of infection... As mentioned in my previous post, I consider those waves to have been self-limiting or seasonally limited. Rather, in the reputed aftermath of the pandemic and especially since the booster vaccination campaigns, we have witnessed a “flattened” BUT near-continuous low-level rolling wave of excess death instead.
Pandemic Prophets
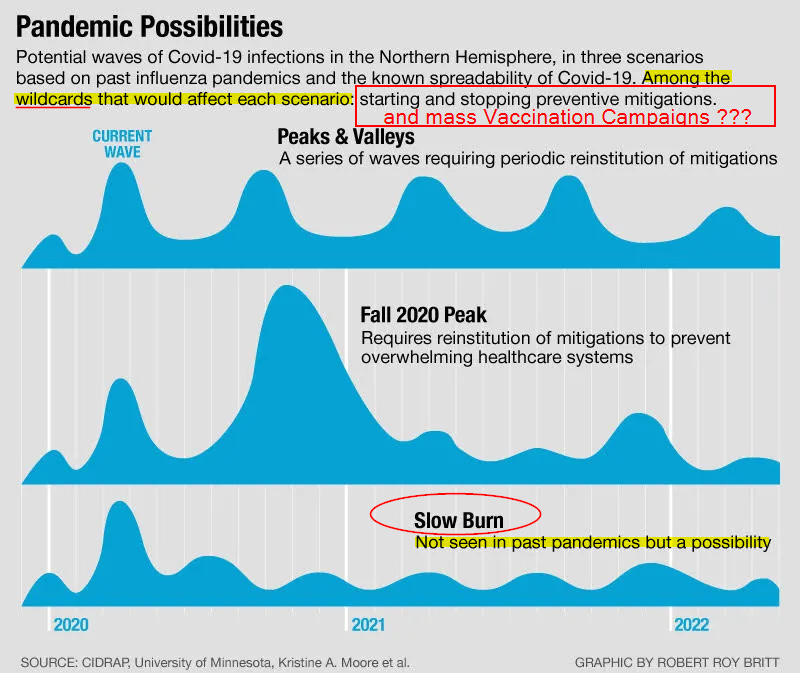
As mentioned in the sub-heading, time is a great revealer. The following paper reports the projections made in Spring 2020 by a working group, The Center for Infectious Disease Research and Policy (CIDRAP), at the University of Minnesota, which I linked to in my “Wuhan Waves vs Spanish Flu” post. The paper is entitled, “Part 1: The Future of the COVID-19 Pandemic: Lessons Learned from Pandemic Influenza”. One of the authors, Dr. Lipsitch, is the director of the Center for Communicable Disease Dynamics, Department of Epidemiology, Harvard TH Chan School of Public Health. Another, Dr. Osterholm, is director of CIDRAP and also a member of the Council on Foreign Relations and went on to join both the Biden administration’s COVID-19 Advisory Board and the National Science Advisory Board on Biosecurity (NSABB). So we are talking heavy-hitters from the mainstream of Epidemiology.
This paper was released 30 April 2020 in the eye of the initial Covid-19 storm in America when some European countries were already seeing their first wave abate. What had the experts to say during the first wave of SARS-CoV-2 in the days when full-blown pandemic hysteria was not yet fully-formed? In a section headed “Key Lessons From Past Influenza Pandemics” the working group had the following to say (all emphasis mine):
Key Lessons From Past Influenza Pandemics
Of eight major pandemics that have occurred since the early 1700s, no clear seasonal pattern emerged for most.
…
The course of these pandemics was not substantially influenced by a vaccination campaign, except for the 2009- 10 pandemic, during which vaccine initially became available in the United States about 6 months after the onset of the pandemic, although substantial quantities of vaccine were not available until after the pandemic had peaked in most parts of the country. One report estimated that the vaccination program prevented 700,000 to 1,500,000 clinical cases, 4,000 to 10,000 hospitalizations, and 200 to 500 deaths in the United States (Borse 2013).
Ah, yes, the Great Swine Flu Pandemic of 2009 - LOL! In other words, the epidemic wave was falling just fine all on its own, but vaccines were administered as quickly as possible AFTER the “pandemic” had peaked - sound familiar? Models were then used to estimate how many cases had been prevented, hospitalisations avoided, and how many lives saved. By the way, 200~500 deaths saved is only ~1% of normal annual flu season deaths in the USA, as estimated by the CDC.
Key points from observing the epidemiology of past influenza pandemics that may provide insight into the COVID-19 pandemic include the following. First, the length of the pandemic will likely be 18 to 24 months, as herd immunity gradually develops in the human population. This will take time, since limited serosurveillance data available to date suggest that a relatively small fraction of the population has been infected and infection rates likely vary substantially by geographic area. Given the transmissibility of SARS-CoV-2, 60% to 70% of the population may need to be immune to reach a critical threshold of herd immunity to halt the pandemic (Kwok 2020).
This may be complicated by the fact that we don’t yet know the duration of immunity to natural SARS-CoV-2 infection (it could be as short as a few months or as long as several years). Based on seasonal coronaviruses, we can anticipate that even if immunity declines after exposure, there may still be some protection against disease severity and reduced contagiousness, but this remains to be assessed for SARS-CoV-2. The course of the pandemic also could be influenced by a vaccine; however, a vaccine will likely not be available until at least sometime in 2021. And we don’t know what kinds of challenges could arise during vaccine development that could delay the timeline.
Lots to unpack. Although the paper is largely speculative in nature, and although the authors genuflectingly pay obeisance to the sanctity of vaccines, it is insightful to regard how epidemiologists could much more openly state their considered opinions about Covid-19 before the entire debate became insanely politicised. Evidently, the collective court of the professional managerial class had not yet proclaimed the acceptable bounds of discussion. “Herd immunity” could still be discussed in connection with infection-conferred immunity. Vaccines were not expected to imminently rescue humanity, and one could still openly opine that infection-conferred immunity could presumably last anywhere from a few months right up to several years. And even if immunity declined after exposure, experts anticipated there could still be some protection against disease severity and reduced contagiousnes. All this could be said by totally mainstream epidemiologitsts in April 2020 during the first wave.
But this was before the narrative coalesced behind the miraculous (95% effective!) vaccines later in the year. Before the approved prophets of science received patronage from the MSM to spout the approved “expert” prophecies from newsroom pulpits. And before any “fringe” voices were banished to the wilderness from the temple of tv-epidemiology broadcasting for the faithful followers of “THE Science”.
Pandemic Prophecies
Without even knowing this was a recognised epimiological thing, I have long been using the analogy of forest fires and the expression “a low-level burn” in previous posts and tweets. Well, it both is and isn’t a recognised thing because it was - until COVID-19 - a theoretical concept not yet observed in practice. From the (CIDRAP) paper (all emphasis mine):
Scenario 3: The first wave of COVID-19 in spring 2020 is followed by a “slow burn” of ongoing transmission and case occurrence, but without a clear wave pattern. Again, this pattern may vary somewhat geographically and may be influenced by the degree of mitigation measures in place in various areas. While this third pattern was not seen with past influenza pandemics, it remains a possibility for COVID-19. This third scenario likely would not require the reinstitution of mitigation measures, although cases and deaths will continue to occur.
I now argue that what we have seen emerge with the unfolding of time is actually a mix of all three scenarios above. As in scenario 2, the initial waves of Covid infections in 2020 increased from spring to autum, and then winter. As in scenario 1, 2020 and 2021 saw deep valleys following their respective spring and winter peak, in fact valleys in which cases dropped to extremely low levels. The start of the pandemic thus followed a similar pattern to the Spanish Flu 1918-19. However, 2022 has seen the third, and previously not seen, scenario where transmission, cases, and deaths are ongoing. Whether it is without a clear pattern or not, is debatable, but: the SLOW BURN has arrived.
True Trends in Bad Data
There are many, many, criticisms that can be made about some of the data collection and processing practices of the various public health authorities around the world during the pandemic, however, if done consistently so, we can at the very least recognise trends within “bad” data which time-series reveal. We cannot say if the magnitude is correct, or even definitively pin the effect down to a specific time (there may be delay effects, etc.); and conclusively identifying the cause may also not be possible (correlation vs causation); BUT the data can still provide clear signals of trends and changes in trends.
This was something I noticed previously while reading T. Coddington’s substack, I Numero. He had processed the Covid-19 incidence rates by vaccine status for England and had proceeded to update this as the weekly surveillance reports were issued. The imperfect data Public Health England data collected and processed consistently (mostly) on the same imperfect basis, revealed genuine trends over time. At the end of 2021, the resulting graphs clearly showed a shifting trend in ratios of the vaccinated:unvaccinated incidences broken out by the various age groups. Without getting bogged down in cohort confounders such as a health user bias, or correlations regarding booster campaigns, waning efficacies, increased natural immunity, or the rise of Omicron, one could still clearly recognise a shifting trend in the data at the end of [EDIT: 2021] in England and elsewhere.
England - Data Trends
Below is a composite graph I have cut and pasted together from various graphs for England available from the official UK government website for data and insights on coronavirus (COVID-19) coronavirus.data.gov.uk. Please note the different scales:
Number of PCR Tests are in millions (per 7-day period);
Test Positivity (right axis) is a percentage (per 7-day period);
Hospitalisations (daily);
Deaths (daily).
Note, I have omitted the infamous “Cases” metric (which is simply the product of positivity and number of tests featured below). Apart from the nebulous nature of what a confirmed case actually means, I contend the dramatic variability in number of tests renders cases an inconsistent and thus less useful metric than positivity. (Please see cm27874’s post Baselines and Bootstrap for a more rigorous statistical treatment of positivity versus test numbers and the probable underreporting of cases in the German data.)
PCR Test Positivity
Skipping over the discussion, for now, of whether “Deaths within 28 days of a positive PCR test” is a meaningful metric and likewise “Patients admitted to hospital with a positive PCR test” - that is the way they have done it, that’s the data we have and it can still reveal signals in trends over time. For example, we can clearly see that peaks in hospitalisations correlate with every peak in test positivity but less consistently so with numbers of tests performed. Regardless of whether these hospitalisations are with or from Covid, I consider positivity a very good proxy for the true incidence rate.
At first it may not be surprising that peaks in “Deaths within 28 days of positive test” also correlate with a lag to peaks in positivity and Covid hospitalisations, however this does lend some credence to the legitimacy of the hospitalisation figures (at least since June 2021). Or should we assume there could be an underlying correlation between hospitalisations for any cause (if they were not truly for Covid) and death within 28 days? Again, at least we have consistency in the data collection, so we can recognise true trends even if the choice of categorisation is questionable.
Deep Valleys
Among the wildcards that would affect each scenario: stopping and starting the mitigations
- CIDRAP, April 2020
Without any vaccines in the first year of the pandemic cases fell sharply after the first wave. By mitigations, the CIDRAP group meant non-pharmaceutical interventions such as masking, social distancing, working from home, school closures, lockdowns, etc. I challenge anyone to show the distinctly similar sharp fall in cases after the winter wave in early 2021 had anything to do with the restrictions or vaccines. The typical scenarios seen repeated around the world were authorities hesitating and deliberating as cases rose, only to introduce lockdowns and restrictions after cases had peaked or alternatively for cases to subsequently rise regardless, with winter ‘21/’22 a prime example. See also many fine posts on this by Joel Smalley explaining Gompertz curves and the typical natural decline of epidemic waves.
Despite millions of tests conducted weekly in the summer of 2020 and spring of 2021 postivity rates fell to less than 1% - this corresponded to less than 50 and 80 hospitalistions per week respectively and deaths fell to single digits. At such high testing rates and with such low positivity it is very possible that even of these few cases some must also have been false positives when the prevalence was so low.
Slow Burn
The course of the pandemic also could be influenced by a vaccine; however, a vaccine will likely not be available until at least sometime in 2021.
- CIDRAP, April 2020
Staying with England’s data, positivity slowly began its renewed ascent in late May, after the early 2021 vaccine campaign. This rising trend was observable 2 months before the UK ‘s official Freedom Day 19 July and its lifting of remaining restrictions. Admittedly, 17 May brought the following loosening of restrictions (see Timeline of UK government coronavirus lockdowns and measures, March 2020 to December 2021):
Limit of 30 people allowed to mix outdoors.
‘Rule of six’ or two households allowed for indoor social gatherings.
Indoor venues will reopen, including pubs, restaurants, cinemas.
Up to 10,000 spectators can attend the very largest outdoor-seated venues like football stadiums.
Nevertheless, I remain puzzled and troubled by the summer outbreak in ‘21 especially as there was no summer oubreak in ‘20 in the absence of restrictions, vaccines, and with much less natural immunity in the community, all of which suggesting ample susceptible hosts for the virus. What is the difference between summer ‘21 and summer ‘20?
Positivity did not dip below 10% again until April 2022, TEN months later. After the initial vaccination campaign and lifting of restrictions, SARS-CoV-2 spread unhindered throughout almost the entire population from summer ‘21 through autumn and winter ‘21/’22. If 10% positivity was representative of the overall population, then 10 sustained months could equate to the whole population!
Apart from the very sharp spikes in positivity of the waves during December ‘21 and March ‘22 which correspond to the first Omicron waves, and a brief dip below 4% in May 2022, positivity has remained roughly between 5~10% ever since summer ‘21.
Vaccine Doses vs Variants
Following three of the pandemics that have occurred since 1900, the pandemic influenza A strain gradually became more human-adapted and replaced the predominant seasonally circulating influenza virus to become the main seasonal influenza A strain identified each year. - CIDRAP, April 2020
Below is a graph I have created showing PCR Test positivity (left axis), this time with both variant proportion (a percentage - right axis) visible as waves and also the vaccine dose rollouts shown as a cumulative percentage (right axis) for the over 12 population. I have tried to glean some further insights from the correlations between variant waves and the test positivity curve but it remains inconclusive. (Note, there was a pre-Alpha variant wave that explains the smaller peak preceding Alpha, however I haven’t found the data to plot that variant.)
Summer ‘21 again sticks out because the Delta wave did not cause an immediate rise in test positivity, unlike the immediately preceding Alpha wave and subsequent Omicron waves, AND that positivity did not fall significantly after the Delta variant peaked. This needs reiterating: with reportedly extremely few cases circulating in March-April-May, Delta became the dominant variant BUT did not trigger an outbreak of widescale infections until late May, which is wholly atypical for respiratory viral infections in the UK.
Recall, the UK's prioritised rollout involved vaccinating as many as possible first with the 1st dose with a longer period, before subsequently ramping up the 2nd dose rollout. Delta’s rise to predominant variant started in April shortly after the rollout of the 2nd dose but positivity lagged a full 2 months behind. Is this indicative of some early protection against infection? I doubt it could be indicative of vaccinees having untested asymptomatic infections because testing levels remained very high (see first graph).
Just as the Delta wave followed the 2nd dose rollout, the first Omicron wave followed the 3rd dose/booster rollout and positivity shot up with Omicron’s rise to dominance. There had been another Delta variant slowly making in-roads but this was rapidly out-competed by Omicron in December. How strong is the corellation with the booster campaign? Note also how positivity fell sharply after the first dominant Omicron variant (BA.1) peaked only to climb sharply again with the subsequent longer Omicron variant (BA.2) in Spring ‘22 (this time despite much reduced testing levels). Thereafter the correlation between test positivity and variants weakens as there are three further peaks of positivity/hospitalistions/covid-deaths (see previous graphic) but only two distinct peaks of a dominant variant.
Interestingly, in 2023 there no longer seems to be a single overwhelmingly dominant variant as was previously the case, though in December ‘22 there was already greater variety establishing.
Inflection Points
First, the length of the pandemic will likely be 18 to 24 months, as herd immunity gradually develops in the human population.
- CIDRAP, April 2020
A 24 month pandemic would have corresponded to March 2022 and yet April 2022, seems to have been an inflection point for the the pandemic in Europe. One could also argue the slow burn first kicked in here but that still leaves the unusual sustained summer-autumn spread in 2021 inadequately unexplained. Below is a very interesting graphic from a twitter thread by Martin Sauter a German physicist. He has used publicly available data at population level to graph monthly excess mortality percentage for European countries against vaccine dose percentage uptake. Note the inflection from March to April 2022:
Based on the population-level data, higher vaccination uptake correlated with less excess death in winter 2021 in Europe BUT from April 2022 onward it correlates with higher excess death rates. This corresponds with both the onset of the unusual pattern of oscillating waves of positivity seen since April and also the sustained unseasonal excess deaths above and beyond those attributed to Covid.
This inflection also correlates with Omicron BA.2 dominance and/or waning protection after the booster campaign - for example, England’s booster campaign began the start of October, while Germany’s later in November. I feel like this is a chicken-egg problem trying to determine causality - what came first? Did boosters create selective pressure promoting the vaccine escaping Omicron variants? Or was it simply a case of any booster protection waning over time allowing a new variant to run rampant? Or, could the boostered be suffering from more than waning protection but rather a form of immune imprinting or immune suppression? See Igor Chudov and Rintra Radagast’s posts for more on this possible phenomenon.
MSM Explanations
The leading mainstream theories which try to explain away the unusual excess deaths data seem to be as follows:
Covid-19 and long-term effects, i.e. the pandemic is not over
Missed or delayed treatments from 2020 and 2021, e.g. cancers, cardio related, etc.
Increased levels of poor health due to pandemic lockdowns (stress, lack of exercise, poor nutrition, etc.)
Overwhelmed medical services (staff shortages, funding shortages, return of flu and other infectious diseases
Unsurprisingly vaccines are reflexively rejected as having any connection with excess deaths
I hope to examine these in greater detail in a further post.
In the meantime, I leave you with a excerpt from my January post Seasonality Shifts:
Waves that crash - Waves that keep rolling
…could also be likened to a forest fire: the first waves raged furiously, burning through all dry wood available but ultimately exhausted themselves (I do not accept lockdowns or other non-pharmaceutical interventions played any significant role in extinguishing the forest fire curves). However, since summer 2021, a low-level burn has persisted. It did not spike (until last month) and thus failed to trigger screaming MSM panic levels but neither has it subsided to normal pre-pandemic levels. It just keeps burning.…in the reputed aftermath of the pandemic and especially since the booster vaccination campaigns, we have witnessed a “flattened” BUT near-continuous low-level rolling wave of excess death instead.
Welcome to the Slow Burn
[UPDATE:] As @_Aussie17 admirably linked my last post which was critical of a post of his I would like to point my readers to his Substack, “Pharmafiles by Aussie17”. Aussie is a former industry insider and is currently covering the slow drip of bad news data releases from many countries for 2022 as well as offering great insights on the pharma industry and their standard operating procedures:
As ever, I appreciate any and all feedback - let me know if you think I have missed something! And please share my articles if you think others would appreciate them:
Witzbold is @_shloka on TWITTER










Great summary of the state of affairs. Thanks for the mention! I don't know why Gompertz does not get more consideration. It is a well-established Phenomenon and not at all difficult to apply.
I wonder why Germany in particular is suffering from so many excess deaths? When the 'pandemic' first hit, compared to England, they got off surprisingly lightly. This might be because they murdered less old folk with Midazolam or it might be because of Karl Friston's 'immunological dark matter', or a combination of both. It does suggest though that 'vaccinating' a population who already have a high degree of pre-existing immunity is not such a good idea.
https://www.theguardian.com/world/2020/may/31/covid-19-expert-karl-friston-germany-may-have-more-immunological-dark-matter